
Brenden Macias
Owner of Key CPR and a Certified Instructor
The Ultimate Guide to CPR: Performing Chest Compressions (Infant|Child|Adult) – UPDATED 2019
- October 14, 2019
- , 1:15 am
- , The Ultimate Guide to CPR
Sharing is Caring —>
The Importance of Effective Chest Compressions
Chest compressions are a crucial element to Full CPR and the only component of Hands-Only CPR. If chest compressions are not performed adequately circulation will suffer and may not be effective at all. If chest compressions are ineffective, CPR will be ineffective. There are some important things to know about chest compressions in order to perform them effectively and efficiently.
How Do CPR Chest Compressions Work?
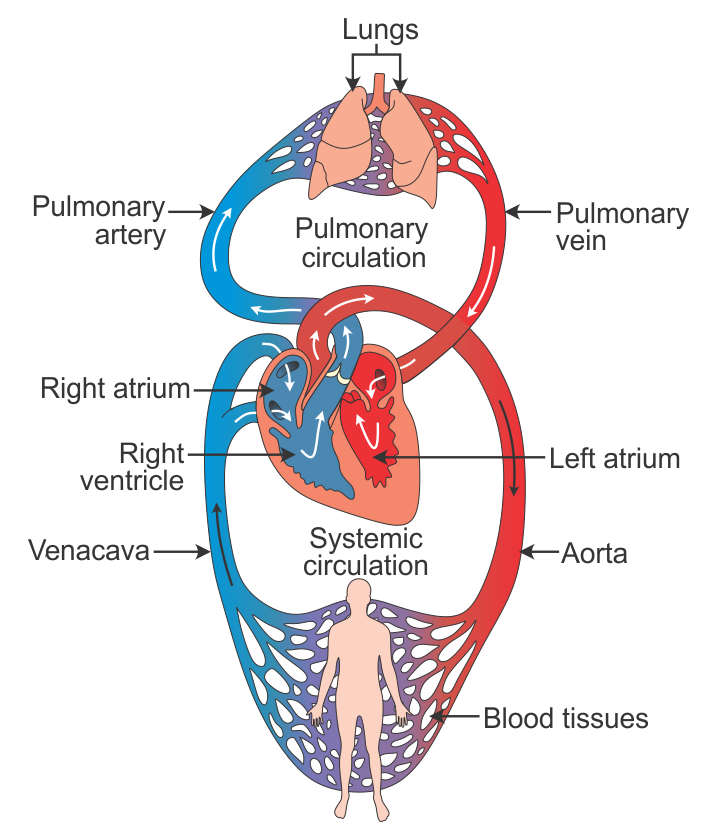
If someone is in cardiac arrest their heart is either not beating or beating too ineffectively to circulate blood to the brain and other vital organs. Chest compressions squeeze a person’s heart in order to manually pump the heart and circulate blood to the body. The valves in the heart only allow the blood to flow through the heart in one direction. When the chest is allowed to return to its normal position (in between compressions) the heart refills with blood. A series of effective chest compressions can keep a person viable until help arrives and can even get the heart beating again on its own, also known as the achievement of ROSC (return of spontaneous circulation).

Getting Someone Ready For CPR
A person needs to be on a firm flat surface for chest compressions to be effective. A bed, couch, or crib would NOT be considered a firm flat surface (unless they have a CPR mode or a CPR board is used). For an infant a table, desk, or countertop works best because providing infant CPR can be easier from a standing position, but the floor can be used if those are not available. Adults and children should be placed on the floor before starting CPR.
CPR Hand Placement For Infants, Children And Adults
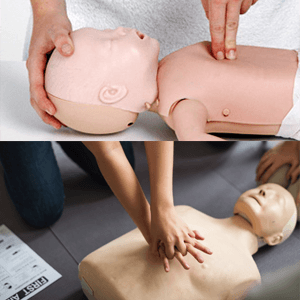
Infants (under the age of 1): Place two fingers in the center of the infant’s chest just below the nipple line using your hand closest to the infant’s feet. The other hand should be placed on the infant’s forehead to brace the infant’s head from striking the firm flat surface you have them on when doing compressions.
Children and adults (1+ years old): Place the heel of your palm in the center of the chest in the lower part of the sternum. Overlay your other hand and interlock your fingers. Keep your fingers up off the chest to concentrate your power to the heel of your palm. Lock out your elbows and get your shoulders up over your hands. For smaller children you may only need to use one hand to perform compressions, which limits your strength a bit.
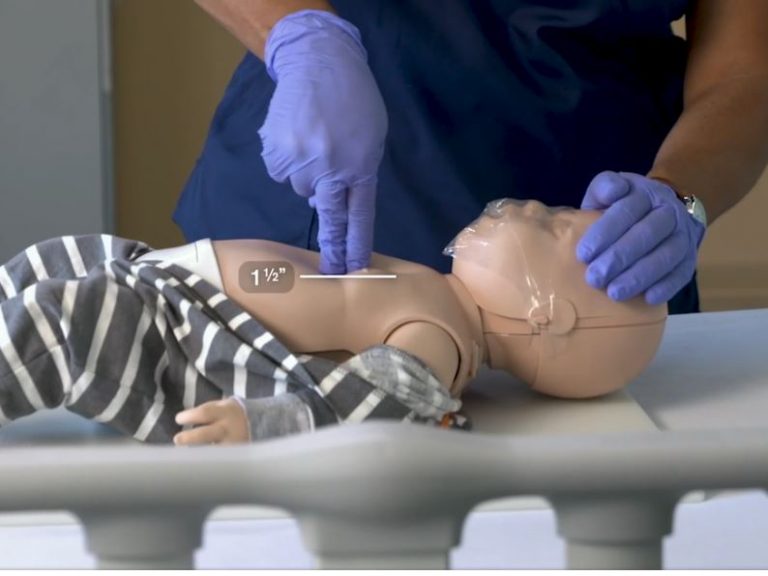
Chest Compression Depth For Infants, Children And Adults
- Infants (under the age of 1): Compress to a depth of about 1.5” using the two-finger compression technique.
- Children (1 to 12 years old): Compress to a depth of about 2”. Use either the two-hand compression technique or the one-hand compression technique for smaller children.
- Adults (12+ years old): Compress to a depth of at least 2” but no more than 2.4″ using the two-hand compression technique.
Proper Rate Of CPR Chest Compressions For Infants, Children And Adults
The rate of compressions is the same for a person of any age, which is 100-120 compressions per minute. Push hard and fast. Use your body weight to help with the compressions. Your elbows should be straight. Bending your elbows will cause you to do “push-up style” compressions, which are very tiring and not nearly as effective. The chest should be allowed to rise completely in between compressions, which allows the heart to refill with blood before the next compression. Counting aload (i.e. 1-and-2-and-3-and-4-and….) is great way to keep the right pace and your count, if performing Full CPR. Another technique that is used, often with Hands-Only CPR, is to choose a song between 100-120 bpm and perform chest compressions to the beat of the music in your head or aloud.


High Performance Chest Compression Tip
Performing chest compressions can be exhausting. When you get tired the quality of your chest compressions decreases. To combat this, you should find others that can help you to perform CPR. Trade off performing CPR every couple of minutes (about 5 cycles of full CPR). Trade off sooner if necessary. Giving each provider time to rest and stay fresh helps to keep chest compression quality high which gives the person needing CPR a better chance of survival.
Hands-Only CPR vs Full CPR
Full CPR is a combination of 30 chest compressions and 2 rescue breaths, regardless of age. If doing Hands-Only (Compression-Only) CPR rescue breaths can be omitted. Full CPR should be used if trained to do so and you can perform Full CPR without endangering yourself. Use of PPE (latex free gloves and breathing barriers as applicable) is recommended. If you are unable or unwilling to perform the rescue breaths (aka mouth-to-mouth) then Hands-Only CPR should be used as an alternate technique. Hands-Only CPR has been shown to be very effective, especially with adults. Some studies have shown that survival rates do drop for infants and children with Hands-Only CPR in comparison to Full CPR.

Can Ribs Break When Performing CPR Chest Compressions?
It is possible to break or fracture ribs when performing chest compressions. For people with brittle bones breaking ribs is very likely. Although injuring someone is not the goal of CPR, it’s important to note that someone needing CPR is in cardiac arrest and would likely die without CPR. If you hear, or feel, something that might be ribs breaking DO NOT STOP CPR.
When Should You Stop Performing CPR?
Continue providing CPR until you see an obvious sign of life, EMS personnel arrive and take over, the scene becomes unsafe, you are too tired to continue, or an AED is available and you are training in using one.

Sharing is Caring —>

